High Salt Intake Linked to Premature Vascular Aging and Immune System Dysfunction According to New Preclinical Research

New scientific evidence has identified a complex biological chain reaction that suggests a high-sodium diet may do more than just raise blood pressure; it may actively trick the immune system into prematurely aging the body’s blood vessels. A preclinical study recently published in the Journal of the American Heart Association has shed light on how excess salt consumption triggers a state of cellular "senescence," a form of biological stagnation where cells stop dividing and begin emitting harmful inflammatory signals. Conducted by researchers at the University of South Alabama, the study provides a granular look at the molecular mechanisms of cardiovascular decay, suggesting that the damage caused by salt is mediated by the body’s own immune response rather than the direct abrasive effect of sodium on the vascular lining.
For decades, the medical community has recognized the direct correlation between high salt intake and hypertension. However, this new research moves beyond the traditional understanding of fluid retention and arterial pressure, focusing instead on the cellular health of the endothelium—the thin membrane that lines the inside of the heart and blood vessels. By observing the physiological changes in mice subjected to a high-salt diet, the research team discovered that the deterioration of blood vessel function occurs with alarming speed, manifesting in as little as four weeks.
The Mechanism of Cellular Senescence
The core of the study’s findings lies in the discovery of cellular senescence within the small arteries responsible for regulating blood flow. In a healthy cardiovascular system, the cells lining the blood vessels are dynamic, regularly dividing and maintaining the structural integrity of the vascular wall. When these cells enter a senescent state, often referred to by scientists as "zombie cells," they lose their ability to replicate. More importantly, they begin to secrete a "senescence-associated secretory phenotype" (SASP), a cocktail of inflammatory proteins and growth factors that can degrade the surrounding healthy tissue.
According to the research team, after only one month of high sodium intake, the small arteries in the test subjects lost their ability to relax and dilate. This flexibility is essential for maintaining healthy blood pressure and ensuring that organs receive adequate oxygenated blood. The study found that the senescent cells failed to produce nitric oxide, a critical gaseous signaling molecule that instructs the smooth muscles of the arteries to relax. Without sufficient nitric oxide, the vessels remain in a constricted, rigid state, which is a hallmark of both advanced age and cardiovascular disease.

The Immune System as a Paradoxical Culprit
One of the most surprising revelations of the University of South Alabama study was that salt does not appear to damage blood vessel cells directly. In a controlled laboratory environment, the researchers exposed isolated blood vessel cells directly to high concentrations of salt in a petri dish. Contrary to expectations, these cells showed no immediate signs of damage or premature aging. This led the scientists to conclude that the vascular decay observed in living organisms is the result of a systemic response rather than local toxicity.
The researchers identified a specific messenger molecule within the immune system called interleukin-16 (IL-16) as the primary driver of this process. It appears that high levels of sodium in the bloodstream trigger immune cells to release IL-16. This molecule then acts as a signal, essentially "instructing" the blood vessel cells to enter a state of senescence. This suggests that the cardiovascular damage associated with a salty diet is an unintended consequence of the body’s own defense mechanisms. The immune system, in its attempt to process or respond to the sodium imbalance, inadvertently accelerates the aging process of the circulatory system.
Experimental Reversal Using Senolytic Drugs
In an effort to determine if this salt-induced aging could be reversed, the research team utilized a burgeoning class of medications known as senolytics. These drugs are designed to specifically target and eliminate senescent cells while leaving healthy cells intact. For the study, the researchers used navitoclax, an experimental medication originally developed for cancer treatment.
The results were significant. By administering navitoclax to the mice on a high-salt diet, the researchers were able to clear out the "zombie cells" that had accumulated in the vascular lining. Following the removal of these dysfunctional cells, the remaining healthy tissue was able to restore nearly normal blood vessel function. The arteries regained their elasticity and their ability to produce nitric oxide, effectively reversing the premature aging caused by the sodium-rich diet. This finding has sparked interest in the potential for senolytic therapies to treat or prevent cardiovascular disease in humans, although experts caution that such applications are still years away from clinical reality.
Global Context: The Sodium Crisis
The implications of this study are particularly relevant given the current state of global nutrition. According to the World Health Organization (WHO), the average global salt intake is estimated to be 10.8 grams per day—more than double the WHO’s recommended limit of less than 5 grams of salt per day (approximately one teaspoon). In the United States, the Centers for Disease Control and Prevention (CDC) reports that roughly 90% of Americans aged 2 and older consume too much sodium.
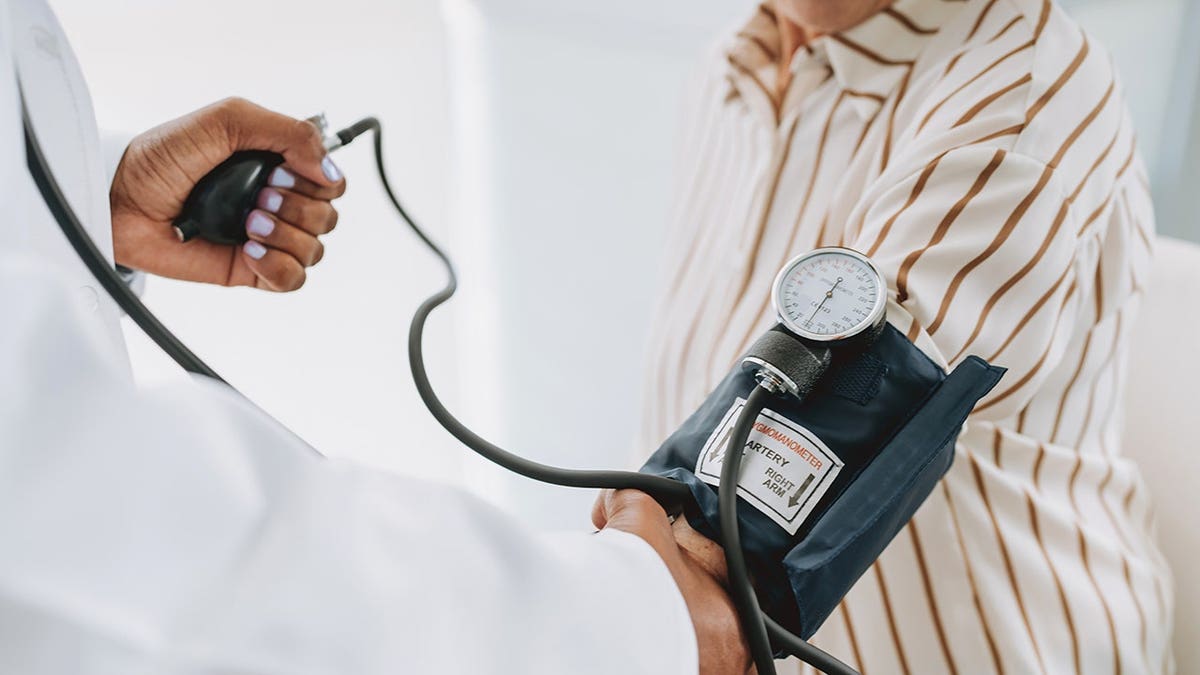
Excessive sodium intake is a primary driver of hypertension, which affects an estimated 1.28 billion adults worldwide. Because hypertension often presents no outward symptoms, it is frequently referred to as the "silent killer." It remains a leading cause of premature death globally, contributing significantly to the incidence of strokes, heart attacks, and kidney failure. The University of South Alabama study adds a new layer of urgency to these statistics, suggesting that the "hidden" damage of salt—cellular aging—may be occurring even before a patient is diagnosed with high blood pressure.
Chronology of Sodium Research and Discovery
The understanding of salt’s impact on the body has evolved significantly over the last century:
- Early 1900s: Researchers first began to link high-salt diets to elevated blood pressure and "hardening of the arteries."
- 1940s: The "Rice-Fruit Diet," extremely low in sodium, was developed by Dr. Walter Kempner to treat malignant hypertension, proving that dietary intervention could reverse heart damage.
- 1970s-1980s: Large-scale epidemiological studies, such as the INTERSALT study, confirmed the relationship between sodium intake and blood pressure across diverse global populations.
- 2000s: Research began to shift toward the endothelium, identifying how salt impairs the production of nitric oxide.
- 2024: The current study identifies IL-16 and cellular senescence as the specific biological pathway through which salt tricks the immune system into aging the vasculature.
Expert Analysis and Potential Implications
While the study’s results are compelling, the research team and independent medical experts emphasize the need for caution. The transition from mouse models to human treatments involves significant hurdles. Biological pathways in rodents do not always mirror those in humans with 100% accuracy, and the safety profile of senolytic drugs like navitoclax is still under intense scrutiny.
"Senolytic drugs are a frontier in anti-aging medicine, but we are not yet at a point where they can be prescribed for dietary-related vascular damage," noted one independent researcher familiar with the study. "Previous human trials involving senolytics have shown mixed results, particularly regarding their effect on arterial plaque stability. We must ensure that clearing out senescent cells doesn’t inadvertently cause other complications in the vascular wall."
Furthermore, the researchers have yet to confirm if the IL-16 pathway is the sole or primary driver of vascular aging in humans. Human biology is influenced by a myriad of factors, including genetics, exercise, and the presence of other chronic conditions like diabetes, which may complicate the immune system’s response to salt.

The Path Forward: Policy and Prevention
The study reinforces the necessity of public health initiatives aimed at reducing sodium consumption. Much of the salt consumed in modern diets does not come from the kitchen salt shaker but is hidden in processed and restaurant foods. In many developed nations, up to 75% of dietary sodium comes from pre-packaged goods such as bread, deli meats, and canned soups.
Public health advocates suggest that if the findings of the South Alabama study are validated in human trials, it could change how doctors approach cardiovascular prevention. Instead of merely managing blood pressure numbers with traditional anti-hypertensives, future treatments might focus on protecting the immune system and preventing cellular senescence.
For now, the medical advice remains steadfast: reducing salt intake is one of the most effective ways to protect cardiovascular health. By avoiding the biological "trickery" that leads to premature vascular aging, individuals can significantly lower their risk of chronic disease and maintain the long-term elasticity and health of their circulatory system. The discovery of the IL-16 pathway provides a new scientific foundation for this advice, proving that a low-salt diet is not just about blood pressure—it is about keeping the body’s internal infrastructure young.




